If your cat has been diagnosed with stomatitis, or feline chronic gingivostomatitis, you are probably dealing with a mix of worry and confusion. This is not a simple dental cleaning situation. Stomatitis causes widespread inflammation of the gums, inner cheeks, and the back of the throat, and cats living with it are often in significant pain even when they do not show it in obvious ways.
At Valley Center Veterinary Clinic, we take a thorough, collaborative approach to stomatitis cases because each cat responds differently and treatment decisions should be made together. As an AAHA-accredited and Cat Friendly Certified practice, we are equipped to perform complete oral exams under anesthesia, full-mouth dental radiographs, and the surgical extractions that are often the most effective path to lasting relief. We walk you through our thought process at every step so you understand what we are recommending and why. Call us at 442-207-4720 or request an appointment to have your cat evaluated.
What Stomatitis Is and Why It Happens
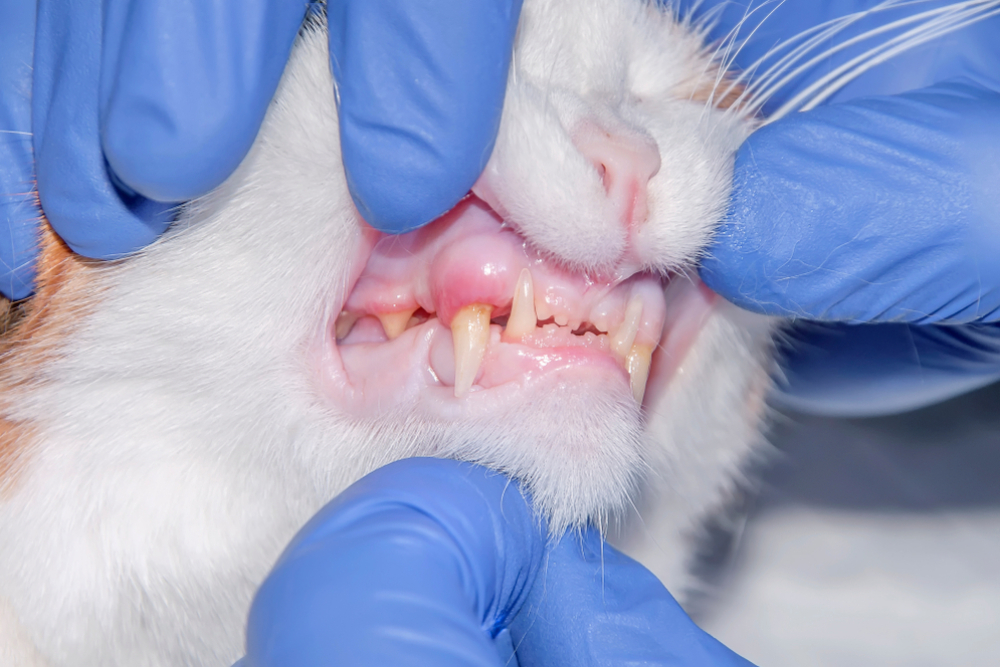
Feline chronic gingivostomatitis (FCGS) is an immune-mediated condition: the cat’s immune system mounts a severely exaggerated response to the plaque bacteria that live on tooth surfaces. The resulting inflammation does not stay confined to the gumline. It spreads across the inner cheeks, the caudal mucosa (the area just behind the last molars), and the tissue surrounding all the teeth, leaving the entire mouth inflamed, ulcerated, and painful.
Some cats also show viral involvement: feline calicivirus and herpesvirus can drive or perpetuate the inflammatory response, which is why viral testing is an important part of the diagnostic workup. FeLV and FIV status also influence prognosis and management. The exact cause of stomatitis is not fully understood, which is one reason treatment must be individualized rather than driven by a single protocol.
Signs and Symptoms of Stomatitis in Cats
What You Might Notice at Home
Cats are expert at concealing pain. By the time visible behavioral changes appear, the condition has often been developing for some time.
Signs worth a same-week call:
- Reduced appetite, or eating only soft food when they previously ate dry kibble
- Weight loss you have noticed over the past weeks or months
- Drooling, sometimes with blood-tinged saliva
- Dropping food mid-chew or eating only on one side
- Pawing at the mouth or face
- Less grooming than usual, particularly around the head
Signs that may indicate the condition is significantly advanced:
- Refusing food entirely despite being hungry (approaching food, sniffing, then walking away)
- Significant weight loss with visible muscle wasting
- Behavioral withdrawal from family interaction
Excessive drooling and food avoidance in cats should prompt a call, not a wait-and-see approach. These signs develop gradually and are easy to dismiss as normal aging, particularly in older cats. Regular preventive exams catch early mucosal changes before they progress, which is one of several reasons routine wellness visits matter for cats throughout their lives.
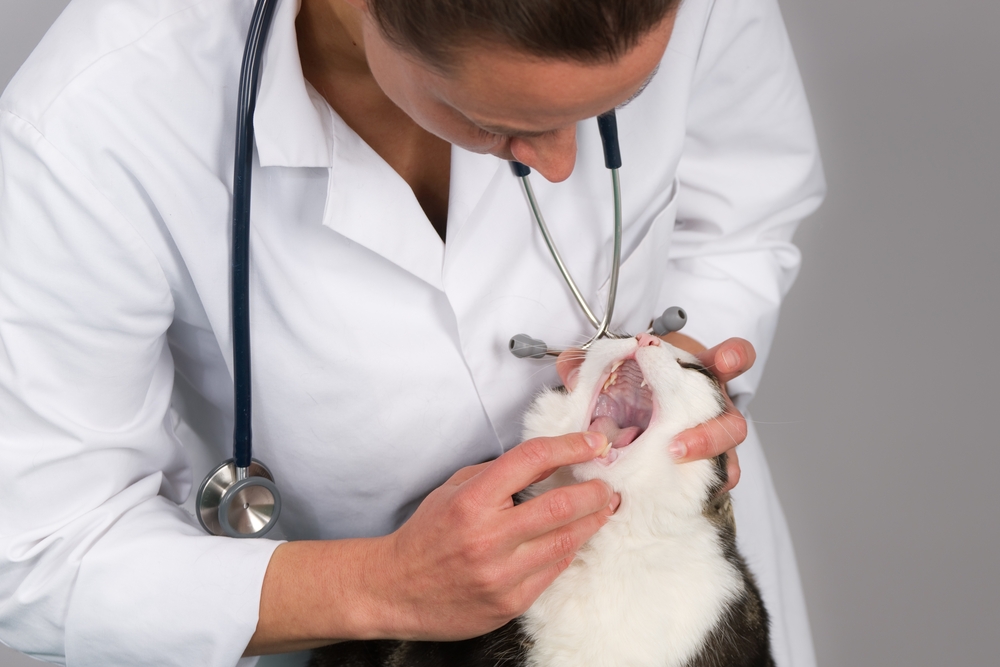
What We Look For During the Clinical Exam
When we evaluate a cat with suspected stomatitis, the oral mucosa is often severely inflamed, ulcerated, and sometimes actively bleeding. The level of pain is usually significant enough that a complete oral exam cannot be performed safely or thoroughly while the cat is awake. Sedation or general anesthesia allows us to fully visualize all surfaces, palpate the affected tissue, and assess the extent of involvement without causing additional distress to a cat already in considerable discomfort.
How We Diagnose Stomatitis
A full evaluation under anesthesia is necessary for an accurate diagnosis:
- Pre-anesthetic bloodwork: organ function assessment before anesthesia
- Complete oral exam: cats with significant oral pain cannot be properly evaluated while awake; anesthesia allows thorough, safe assessment of all tissue surfaces
- Full-mouth dental radiographs: bone loss, retained root fragments, and periapical disease are invisible without radiographs and matter for surgical planning
- Viral testing for feline calicivirus, feline herpesvirus, FeLV, and FIV: viral status directly influences post-operative care and long-term management
Our diagnostics capabilities support this complete workup, and our team explains findings before any treatment begins.
Stomatitis vs. Periodontal Disease (and When to Suspect Something Else)
Distinguishing stomatitis from periodontal disease matters because the two require different approaches, and most stomatitis cats have both simultaneously. Periodontal disease targets the tooth-supporting structures (bone, ligaments, and attachment tissue), while stomatitis spreads throughout the entire oral cavity and does not respond to routine dental cleanings alone. Dental radiographs are the only way to fully assess what is happening beneath the gumline, including root integrity, bone density, and any retained fragments that could be driving ongoing inflammation.
When oral lesions appear unusual or asymmetric, oral cavity tumors must be ruled out before proceeding with stomatitis treatment. Tissue biopsy is the appropriate next step when the appearance does not match what we typically see with stomatitis, particularly when proliferation is one-sided or when a discrete mass is present.
Treatment Pathways
Medical Management and Its Limitations
Anti-inflammatory medications, antibiotics, pain management, and antiviral treatments for confirmed viral involvement form the foundation of medical management. Soft food or appetite stimulants help cats who are struggling to eat comfortably during the diagnostic period, and in severe cases a temporary feeding tube supports nutrition while a longer-term plan is developed.
Medical management is an important bridge, particularly for severely debilitated cats who need nutritional support before surgery. The honest answer is that medication does not address the underlying immune trigger and rarely produces lasting remission as a standalone approach. It tends to become less effective as the disease progresses, and prolonged use of immunosuppressives carries risks that can reduce the chances of a good surgical outcome later.
Full-Mouth Extraction: The Most Effective Treatment
Full-mouth tooth extraction removes the plaque-retaining surfaces that trigger the immune response. Studies consistently show 60 to 80 percent of cats achieve substantial improvement or complete resolution after full-mouth extraction. Earlier intervention, before extensive mucosal scarring, produces the highest resolution rates.
Complete root removal is essential. Retained root fragments are one of the leading reasons inflammation persists after surgery, which is why post-extraction radiographs are taken at the same procedure to confirm everything has been removed. During the surgery, supportive measures include local nerve blocks for intraoperative and post-operative pain control, continuous anesthetic monitoring, and therapeutic laser application at the surgical sites to reduce inflammation and support healing.
Anesthesia and dental procedures performed to AAHA-accredited standards form the foundation of safe, complete extraction. Our AAHA-accreditation means we adhere to the highest standards of medical care and patient safety, stay up-to-date on the most recent treatments, and will take the time to explain every step. We also are fully transparent about our pricing, even for dental care. We want you to feel confident and comfortable with the care your cat receives and the plan for treatment.
Advanced Options for Non-Responding Cats
Some cats, particularly those with active calicivirus involvement or prolonged disease before surgical intervention, continue to have significant inflammation after full-mouth extraction. Newer advanced options for these cases include:
- Adipose-derived mesenchymal stem cell therapy: uses the cat’s own fat-derived stem cells to modulate the immune response. Has produced meaningful results in cats who did not respond to standard approaches.
- MSC secretome: a cell-free preparation of the bioactive factors stem cells produce.
- Cryotherapy: targeted application of extreme cold to affected oral tissue.
- Advanced antiviral and immunomodulatory protocols for confirmed viral-driven cases.
We discuss referral for these options when standard treatment does not produce the expected improvement.
What Recovery Looks Like After Full-Mouth Extraction
The question nearly every family asks before agreeing to full-mouth extraction is: how will my cat eat without teeth?
Most cats adapt remarkably well. Within a few weeks of recovering from the significant oral pain they were living with before surgery, most cats eat with more enthusiasm than before. They manage wet food with their gums, and many eventually eat dry food as well. The transformation families describe most consistently is a cat who seems comfortable for the first time in months or years.
A typical recovery looks like:
- First 7 to 10 days: prescription pain management, antibiotics if indicated, and soft or canned food only. Activity is naturally reduced; rest is the priority.
- Two-week recheck: evaluation of the surgical sites and a check that healing is progressing as expected.
- Two to four weeks out: most cats are eating with noticeably more enthusiasm, grooming returns to normal, and personality changes from chronic pain begin to resolve.
- Long-term follow-up: for cats with calicivirus carrier status, continued immunomodulatory therapy may be appropriate. For cats without viral involvement, many need no ongoing medication at all.
Our Cat Friendly Certified approach ensures every part of the visit, including recovery discussions, happens in a way that keeps your cat as comfortable as possible.
Long-Term Prognosis: What Influences Outcomes
Early treatment consistently produces the best results. The factors that most shape prognosis include:
- Duration of disease before treatment: longer disease history means more established mucosal scarring and a lower rate of complete resolution
- Completeness of extraction: retained root fragments are a leading cause of persistent inflammation; post-extraction radiographs confirm complete removal
- Viral carrier status: active calicivirus involvement may extend recovery and require ongoing management
- Individual immune response: some cats need continued anti-inflammatory therapy even after successful extraction. This is not a treatment failure but a management reality for their specific immune presentation.
Even cats needing ongoing medication after surgery typically experience a significant reduction in pain and inflammation and return to normal daily behavior, which is the outcome that matters most.
Maintaining Oral Health for Cats Without Stomatitis
For cats without stomatitis, consistent at-home habits and professional care prevent significant dental health problems and catch early issues before they progress. For cats with stomatitis, good dental care can help slow progression of the disease but won’t stop it completely. Annual professional cleanings with full-mouth radiographs are appropriate for most cats. Between visits, the right home dental routine depends on what your individual cat will tolerate.
We have several great options from our pharmacy:
- CET enzymatic toothpaste and CET Fingerbrush for cats who tolerate brushing
- Dental wipes for cats who resist brushing
- Dental rinses and water additives for passive daily care
- Dental Care Powder added to food
- Greenies dental treats, ProDen DentalCare bites, and dental diet options
Frequently Asked Questions
Is stomatitis curable?
For many cats, full-mouth extraction produces complete resolution. Others require ongoing medication but at a reduced level and with significantly less pain than before surgery. Outcomes vary, and we discuss realistic expectations based on your cat’s specific presentation before any treatment begins.
How do cats eat without teeth?
Comfortably, for most. Cats do not chew the way humans do; they grasp and shear rather than grind. Most cats just inhale their food instead of chewing, anyway. Wet food is easily managed with gums, and many toothless cats manage dry food as well.
Can stomatitis be managed with medication alone long-term?
For most cats, medication alone provides diminishing returns over time. The disease typically continues to progress, and cats on long-term immunosuppressives carry increased infection risk. Surgery produces more reliable lasting improvement.
Will my cat need lifelong treatment after extraction?
Many cats need no further treatment beyond routine wellness once they have healed. Some need periodic recheck exams or low-dose anti-inflammatory therapy long-term, depending on viral status and individual response. Either way, the day-to-day comfort difference after extraction is dramatic.
A Thorough, Honest Approach
Valley Center Veterinary Clinic’s collaborative care model means you understand the reasoning behind every recommendation before you agree to it. Stomatitis cases are some of the most meaningful we manage because the improvement a cat experiences after effective treatment is genuinely dramatic. The cats who do best are those whose families act early.
Request an appointment or contact us at 442-207-4720 to schedule an oral evaluation for your cat. Our adult cat wellness visits include oral health assessment at every examination.







Leave A Comment